Lifestyle Resources
Health Resources
Medical Resources
Preventive Care
Health and Well-being Support
Resources
Help Center
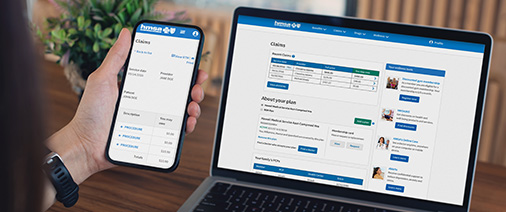
HMSA’s My Account
Manage your plan online with HMSA’s My Account. My Account gives you convenient access to your health plan information.
Contact Us

HMSA Neighborhood Centers
Take control of your health care by getting answers to your questions from someone who knows. Our representatives can help you learn about your bill, make payments, check on a claim, explore well-being resources, or start a new plan.
- Health Plans More
- Well-being More
- Member Discounts More More
- HMSA’s Online Care
- Maternal Health
- Quitting Tobacco & Cravings
- Telehealth
- Health Condition Support and Resources More More
- HMSA Diabetes Prevention Program
- Health Education Workshops
- Mental Health
- Advanced Care Program
- ED Care Pathways Program
- Healthy Living
- High-Risk Pregnancy Program
- Transitions of Care Program
- Help Center More
- Contact
- Employers
- Providers
- About More
- Careers More
- Media Center
- Awards and Scholarships More
- Sitemap
